Types of Bone Fractures: Treatment Options and Recovery
Not all bone fractures are the same. Some are clean breaks that stay within the skin. Others are jagged, shatter the bone into pieces, or pierce through muscle and tissue. A fracture, in clinical terms, refers to a break in the continuity of the bone structure. This can be due to a fall, direct trauma, repetitive stress, or weakened bone due to conditions like osteoporosis. The nature of the fracture determines both how it presents and how it is managed. Knowing the different types of fractures is essential for understanding treatment needs and expected recovery outcomes.
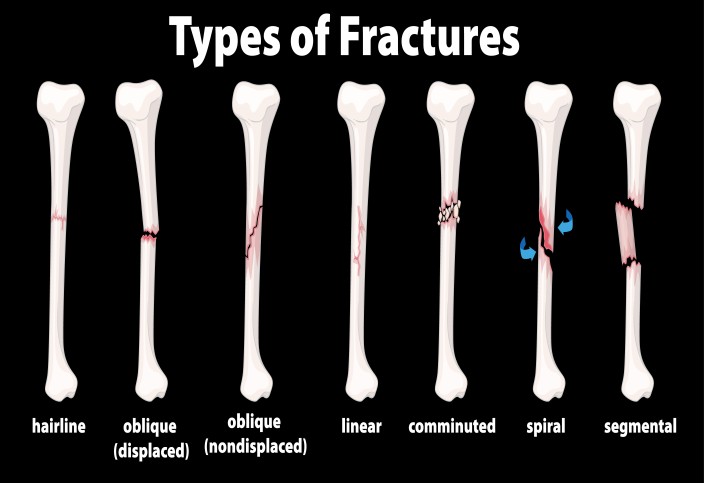
Types of Fractures
Fractures are classified based on the way a bone breaks and whether surrounding tissues are affected. Here are the key types:
Closed (Simple) Fracture
The break occurs inside the body without piercing the skin. It is often detected by swelling or an abnormal shape of the limb.
Open (Compound) Fracture
The bone pierces through the skin. There's a high risk of infection, and these cases require urgent surgical attention.
Transverse Fracture
The bone breaks across in a straight, horizontal line in this case. Transverse fractures are common in high-impact injuries.
Oblique Fracture
The break is diagonal across the bone. It is often caused by a sharp angled force during a fall or sudden movement.
Spiral Fracture
A twisting injury causes the bone to fracture around its shaft, forming a spiral pattern. This is frequently seen in sports injuries.
Comminuted Fracture
The bone breaks into three or more pieces. It is caused by severe trauma, such as road accidents.
Greenstick Fracture
This type is unique to children due to the flexibility of young bones. The bone bends and cracks on one side but doesn't break completely.
Compression Fracture
Most often seen in the spine, particularly in older adults with osteoporosis. The bone is crushed, and the height is reduced.
Impacted Fracture
One part of the bone is driven into another. It often results from falls or sudden compressive forces.
Each of these fracture types requires different strategies for treatment and healing.
What Are The Risk Factors For Fracture?
While anyone can suffer a fracture, some people are more vulnerable due to certain risk factors like:
- Ageing bones: With age, bones naturally lose density and strength and increase fracture susceptibility.
- Osteoporosis: A major cause of fragile bones seen in postmenopausal women and the elderly.
- Previous fractures: A history of bone fractures increases the likelihood of future ones.
- Chronic medical conditions: Disorders like rheumatoid arthritis, thyroid disease, and diabetes can compromise bone health.
- Sedentary lifestyle: Lack of weight-bearing exercise weakens bones over time.
- Certain medications: Long-term use of corticosteroids is an example that can lead to bone loss.
- Nutritional deficiencies: Low calcium or vitamin D levels impair bone regeneration.
- Smoking and alcohol use: Both can reduce bone mineral density, and it can delay healing.
Being aware of these factors helps in early risk identification and prevention through bone health monitoring and lifestyle adjustments.
How are Bone Fractures Treated?
Treatment depends on several factors, such as fracture type, location, alignment, and whether surrounding tissues are affected. Some common treatment options are:
Immobilisation
Using a cast or splint to hold the bone in place while it heals. Best for stable, non-displaced fractures.
Traction
A less common method that uses a steady pulling force to align bone fragments, sometimes used in femoral or spinal injuries.
Surgical Fixation
For complex or open fractures, surgical procedures such as Open Reduction and Internal Fixation (ORIF) are performed. These involve plates, screws, or rods to stabilise the bone.
External Fixation
Metal pins and rods are placed externally to hold the bones in place when the skin and soft tissues are too damaged for internal fixation.
Rehabilitation
Physiotherapy begins after initial healing. It restores joint mobility, rebuilds muscle strength, and prevents stiffness. If the rehab is delayed, it can lead to long-term functional limitations.
Fracture complications like malunion (improper healing), non-union (failure to heal), infections, and nerve injuries make timely treatment critical. Early orthopaedic evaluation prevents these outcomes and helps preserve long-term bone integrity.
What is the Recovery Timeline for fractures?
Healing is not a uniform process. It varies based on the fracture type, age of the patient, presence of other health issues, and how strictly you are following physiotherapy.
- Simple fractures often heal in 6 to 8 weeks.
- Comminuted or open fractures require several months or more due to the complexity of bone and tissue damage.
- Elderly individuals or patients with osteoporosis need prolonged recovery and closer monitoring.
Rehabilitation begins during or after immobilisation. Early mobilisation preserves joint range and prevents stiffness. Strength training, gait training, and balance exercises follow as healing progresses. For hand or wrist fractures, fine motor exercises are important. For lower limb injuries, weight-bearing training and walking re-education might be necessary. Recovery is not just about bone fusion; it’s also about regaining full functionality.
Conclusion
Now that you have read all about bone fractures, you know that they are all different. Their cause, severity, and pattern influence how they’re treated and how long they take to heal. Whether it’s a clean break or a complex injury, timely diagnosis, skilled intervention, and structured rehabilitation are essential to ensure full recovery.
At Hinduja Hospital Khar, our orthopaedic team has comprehensive fracture care from advanced imaging and surgical repair to personalised rehab programs. Book an appointment today and take the next step toward recovery with medical care that prioritises structural healing and long-term function.
Frequently Asked Question (FAQs)
What are the two most common fractures?
The most common fractures are clavicle (collarbone) and distal radius (wrist) fractures. Both are frequently caused by falls or direct trauma and are especially common in sports injuries and among older adults.
What are the 5 stages of fracture healing?
The 5 stages of fracture healing are:
- Hematoma formation
- Granulation tissue development
- Callus formation
- Ossification
- Bone remodelling
Which bone is most likely not to heal properly?
Fractures in the tibia (shinbone) and humerus (upper arm) are most likely to experience delayed healing or nonunion due to limited blood supply or high stress on the bone during recovery.
Submit your query